RPA IMPLEMENTATION - CASE STUDY
ABOUT THE CUSTOMER: One of the leading US health care provider, based out of kentucky & one of the largest hospital operator. Customer specializes in handling specialty & commercial plans. An external vendor was handling the delivery of E2E claims adjudication process. Application landscape consists of web ui based core adjudication with 37+ external & internal interfaces (communicate through webservice calls) and 10+ upstream & downstream applications (including customer information, healthcare plans, provider networks, letter generations, prepay management & financial audits)

OUR CHALLENGES
01.
Finalizing prepay adjustments in outstanding claim payments is performed across 3 applications covering 7 workflows. 12 field auditors are assigned to handle the day workload (200 transactions per person per day)
02.
Based on updated business rules (updated by business users) claims should be prioritized for finalizing the prepay adjustments. Claims prioritization is performed with excel based rules for once in every 2 hours
03.
Present FPR for the customer is 73.24% which is planned to scale up to 84%. This will make sure to address all federal compliances are met and all high priority claims are addressed within the fixed time-line.
SOLUTIONS IMPLEMENTED
01.
SMART BOTS were deployed for handling Claims Suspended due to Prepay Adjustments. 300 Business Rules were addressed while arriving at the claims finalization. Suspended Claims will be retrieved using SQL Queries from the Claims Adjudication platform, specific adjustments were applied to each claim
Complete replacement of 12 member Prepay Audit Team saving 360 hrs of manual effort every week $30K per month)
02.
Developed 2 BOTs with cognitive abilities that will coordinate to prioritize the Claims, One BOT will handle the profile creation process which will read complete claim history (including the dependent claims). The other BOT has the computation of all Business Rules in place which will coordinate & prioritize the Claims accordingly
Improved overall Accuracy, Efficiency and accessibility to Legacy Applications-to retrieve and update data to these systems without any hindrance.
03.
Handling errored out claims requires verification on multiple fronts -including analysis of complex X12 files, EDI transaction history, Claim history, compilation of Member data, Provider data. Errored out Claims are then validated across these factors, corrective measures taken by re-tracking 7 applications and re-process the claims to finalize without manual intervention. 5 SMART BOTS were created to coordinate & perform the complete E2E process.
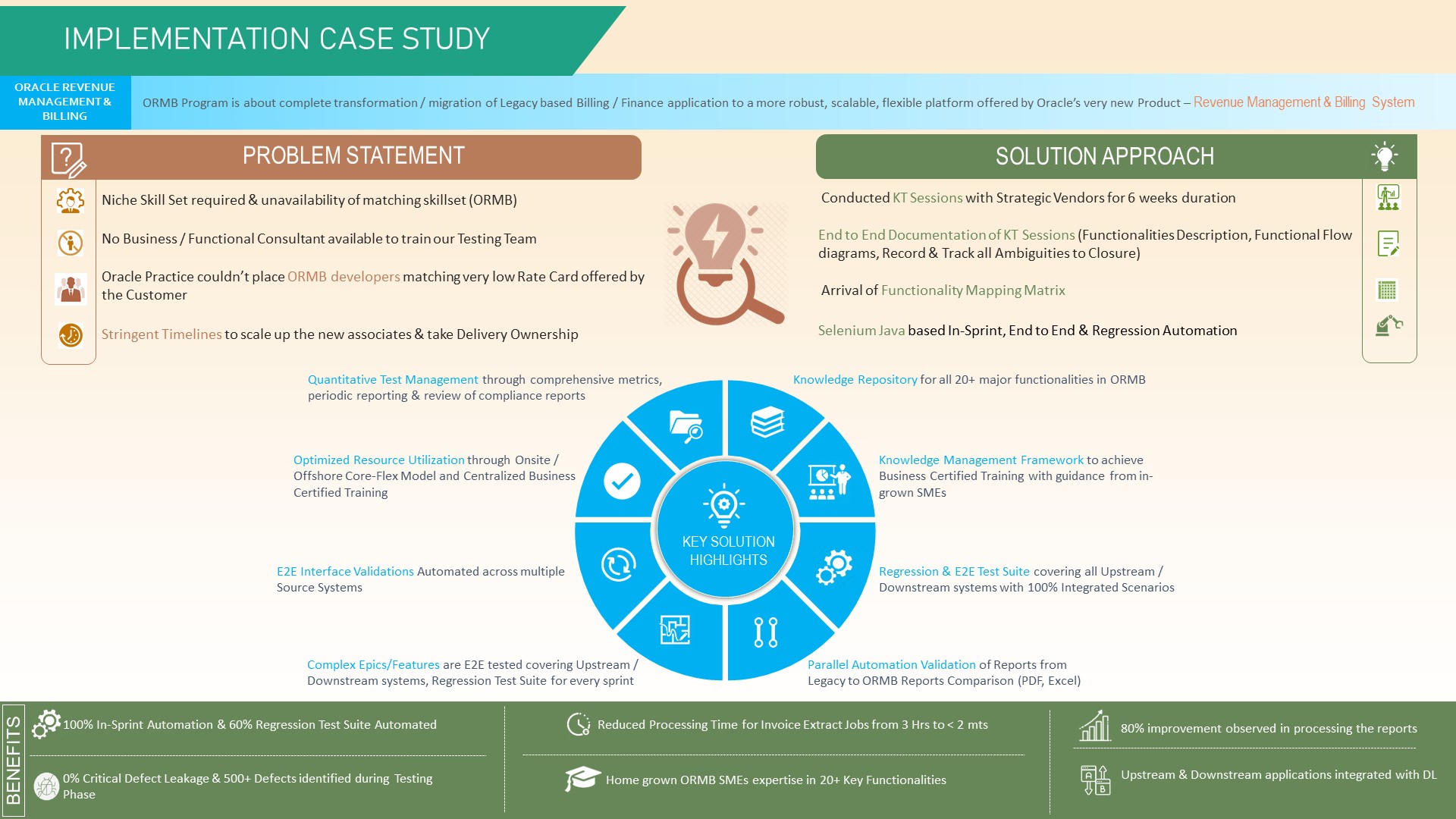
IMPLEMENTATION CASE STUDY
ORACLE REVENUE MANAGEMENT & BILLING?
This Program is about complete transformation/migration of Legacy based Billing System to a more robust, scalable, flexible platform offered by Oracle's very new Product - Revenue Management & Billing System
- Niche Skill Set required & unavailability of matching skillset (ORMB)
- No Business/Functional Consultant available to train our Team
- Oracle Practice couldn’t place ORMB developers matching very low Rate Card offered by customer
- Stringent Timelines to scale up the new associates & take Delivery Ownership
- Conducted KT Sessions with strategic vendors for 6 weeks duration
- End to End Documentation of KT Sessions (Functionalities Description, Functional Flow diagrams, Record & Track all Ambiguities to Closure)
- Arrival of Functionality Mapping Matrix
- Selenium Java based In-Sprint, Regression Automation & E2E Automation
- Quantitative Test Management through comprehensive metrics, periodic reporting & review of compliance reports
- Optimized Resource Utilization through Onsite/ Offshore Core-Flex Model and Centralized Business Certified Training
- E2E Interface Validations Automated across multiple Source Systems
- Complex Epics/Features are E2E tested covering Upstream/ Downstream systems, Regression Test Suite for every sprint
- Parallel Automation Validation of Reports from Legacy to ORMB Reports Comparison (PDF, Excel)
- Regression & E2E Test Suite covering all Upstream/ Downstream systems with 100% Integrated Scenarios
- Knowledge Repository for all 20+ major functionalities
- Knowledge Management Framework to achieve Business Certified Training with guidance from in- grown SMEs